Long COVID Patients Are Waiting Months for Care, and the Problem May Only Get Worse
0 View
Share this Video
- Publish Date:
- 7 February, 2022
- Category:
- Natural Cures
- Video License
- Standard License
- Imported From:
- Youtube
Tags
In March 2020, Laura Fitton, a 50-year-old entrepreneur in Massachusetts, had a high fever, sore throat, gastrointestinal issues, and loss of taste. But at the time, few of those symptoms were linked to COVID-19, so Fitton wasn’t eligible for a test. It took seven more months of persistent symptoms—including brain fog, swollen joints, fast heart rate, chills, and fatigue—for a doctor to order an antibody test. Although the test came back negative—perhaps because of how much time had passed since she had gotten sick—Fitton was relieved that a doctor was finally exploring the possibility of Long COVID, a little-understood condition in which people suffer symptoms long after their acute infection passes.
[time-brightcove not-tgx=”true”]
Two years after her initial illness, getting care is still a battle. She must wait until July for a simple screening call with a Long COVID clinic in Boston, and until this October for a neurologist to walk through the results of tests he ran on her in November 2021. In the meantime, she’s mostly on her own to manage her symptoms, which are still present but have improved significantly since she got vaccinated last year. “I can’t imagine what this is like for somebody who’s in the condition I was in,” she says, “and is just getting stonewalled everywhere.”So many people are suffering from Long COVID that treatment centers can’t keep up. In many ways, that’s understandable: the diagnosis did not exist before 2020. New York City’s Mount Sinai Health System was one of the first places in the country to launch a post-COVID-19 recovery center, in May 2020. By early 2021, many top U.S. hospitals, including the Mayo Clinic, the Cleveland Clinic, and Massachusetts General Hospital, had taken notice and opened their own practices. There is now at least one Long COVID treatment clinic in almost every U.S. state, according to a directory kept by Survivor Corps, a COVID-19 and Long COVID patient-support group.TIME Illustration. Viral cell icon: Getty ImagesAs many Americans begin to wonder if there’s a light at the end of the COVID-19 tunnel, new clinics are continuing to open across the country, an acknowledgment that Long COVID symptoms won’t disappear even if the pandemic fades. After treating long-haulers—the name sometimes given to people who have Long COVID—virtually throughout the pandemic, cardiopulmonary physical therapist Noah Greenspan opened a brick-and-mortar pulmonary-rehab center in New York City in December because, he says, “We need action, not lip service,” to solve the Long COVID problem. Indiana’s Parkview Health also opened a clinic for pediatric Long COVID patients in December, and Madonna Rehabilitation Hospital in Nebraska opened a recovery center the same month.Even with this progress, medical care has not kept pace with the overwhelming needs of patients, given how many people report months-long waits for care or can’t find it at all. With research about Long COVID and its treatment still in its early stages, there is no guarantee of recovery even for those lucky enough to get into a specialty clinic.“I’m pleased to see the growth of the post-COVID care centers,” says Diana Berrent, who founded Survivor Corps after testing positive for COVID-19 in March 2020. But “I’ve yet to see where they are really moving the needle in terms of actually getting people better.”
Read More: Omicron Could Be the Beginning of the End of the COVID-19 Pandemic
It’s not clear how many Long COVID patients there are in the U.S. In 2020, researchers estimated that between 10% and 30% of people with COVID-19 would develop long-term symptoms. That percentage is probably lower among people who have been infected after being vaccinated, given that studies have shown that being vaccinated significantly reduces the odds of developing Long COVID.The U.K. has a better understanding of the scope of the problem. According to data published in January by the U.K. government, about 1.3 million people there said they were living with Long COVID as of December 2021. Estimates vary for the U.S., but authors of a paper published in August 2021 in the New England Journal of Medicine estimated that at least 15 million people in the U.S. would have Long COVID by the pandemic’s end. However, that was published before the emergence of the highly contagious Omicron variant, which has already produced a record-shattering number of cases—some of which are likely to develop into Long COVID.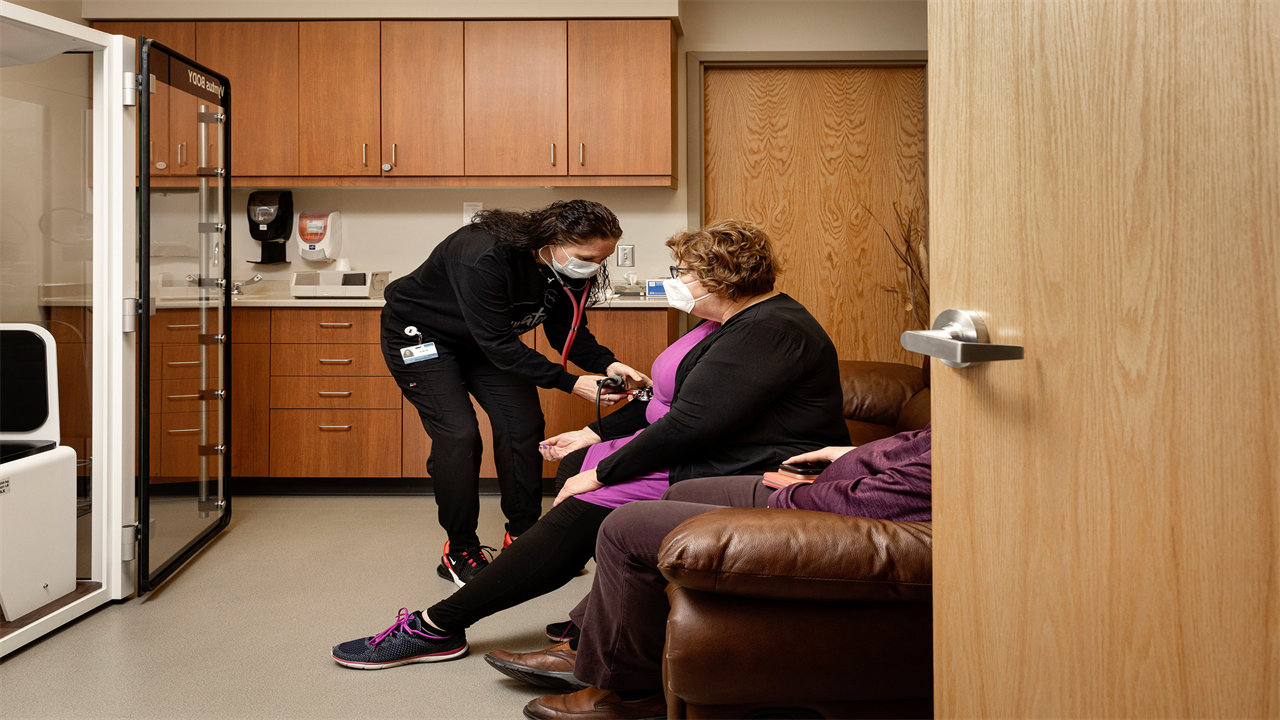
Rebecca Stumpf for TIMEAmber Rausch’s blood pressure is taken during Long COVID testingThe U.S. healthcare system can barely keep up. Because people with Long COVID have reported more than 200 distinct symptoms, they often require care from clinicians in multiple specialties, from pulmonology and neurology to gastroenterology and psychiatry. Stanford’s Post-Acute COVID-19 Syndrome Clinic, for example, tries to use its slim staff most efficiently through a hub-and-spoke model, explains co-director Dr. Linda Geng. Each patient is examined by one of the clinic’s staff physicians and, if necessary, is then referred to a specialist. The clinic analyzes five or six new patients each week, Geng says—but it has a months-long waitlist.To see more patients, the clinic would need not only more physicians, but also more nurses, medical assistants, and billing coordinators, Geng says. That’s no small order, given the personnel shortages that have plagued the industry since before the pandemic. In 2019, the U.S. had an estimated 20,000 fewer doctors than necessary to meet demand. Now, after mass resignations and with rampant staffing issues because of Omicron, hiring extra health care workers is even more challenging.
Read more: What Actually Worries U.S. Doctors About Omicron
Long waits are also partly due to the criteria many clinics require new patients to meet. Many care centers treat only people who had a laboratory-confirmed COVID-19 diagnosis. But many people with lingering symptoms—particularly those who got sick in the spring of 2020, before tests were widely available—never got a positive COVID-19 result.Dr. Brad Nieset, a family-medicine physician, runs one of Montana’s only Long COVID treatment clinics, Benefis Health System’s Post-COVID-19 Recovery Program. He does not require a positive test result from his patients. “No matter what, they called me because there’s a problem,” he says. The clinic has treated about 600 people so far and currently has a waitlist about a month long.To help triage the requests, Nieset begins with a telehealth consultation. Then, when patients come into the clinic—sometimes driving from hundreds of miles away—his team performs a comprehensive physical and mental assessment to decide who can be treated by a primary-care provider, and who needs care from specialists.Long COVID clinics must rely heavily on primary care to meet surging demand, says Dr. Gavin Yamey, associate director for policy at the Duke University Global Health Institute. There aren’t enough specialists, and many people can’t afford their services anyway. “It begins in primary care,” Yamey says. “There needs to be awareness and recognition of the condition, and health care providers need to understand what the care pathway looks like.”The problem is, nobody fully understands how to cure Long COVID. In that regard, it’s similar to other mysterious and complex chronic illnesses like myalgic encephalomyelitis/chronic fatigue syndrome (ME/CFS), chronic Lyme disease, and fibromyalgia. “To be frank,” Geng says, “we don’t have a curative therapy.”Still, people have recovered from Long COVID. Some, like Fitton, improve after vaccination, although experts aren’t sure why it happens; others have damage to a specific organ or an underlying illness that is fairly straightforward to treat; and others simply get better with time.Read More: Can Breakthrough Infections Lead to Long COVID? For an Unlucky Few, Yes
Amber and Mike Rausch, both of whom are 53 and in treatment for Long COVID at the Benefis clinic in Montana, are two such success stories. Both husband and wife caught COVID-19 in late 2020 and experienced symptoms well into 2021: complete exhaustion for Mike and brain fog and excruciating headaches for Amber.
Rebecca Stumpf for TIMEDr. Brad Nieset talks with Mike and Amber Rausch after completing testing for Long COVID symptomsThey were relieved when Mike was referred to the Benefis clinic in the summer of 2021. Starting with Mike’s initial screening call, Amber says, they felt comforted by learning that “we know so much more about COVID and long-haul symptoms than we did at the beginning of the pandemic,” she says. “I just remember [Nieset] giving us so much hope that day.”Nieset’s team noticed during intake screenings that Mike had significant lung damage and started him on nighttime oxygen and a home breathing device called a nebulizer. “I feel 10 times better,” Mike says. “I don’t think I’m quite back to pre-COVID, but I’m 90, 95% there.”Amber also recently started with a slew of assessments, from chest X-rays to cognitive, breathing, and physical-fitness tests, to find the root cause of her symptoms. Like her husband, she has improved with overnight supplemental oxygen.But other patients remain sick for no clear reason, says Dr. Luis Ostrosky-Zeichner, a leader of UTHealth’s post-COVID-19 recovery program in Texas. (The clinic has about 900 current patients and still has a waitlist.) “These patients are sick and they’re symptomatic and we need to take care of them,” Ostrosky-Zeichner says. “But we need to get to the bottom of why are they here?”
Read More:A Year Into the Pandemic, Long COVID Is Still Burdening Patients—and Their Caregivers
The U.S. National Institutes of Health has earmarked more than $1 billion for Long COVID research, but it could be years before those studies produce actionable results. “Consolidating the way we study these patients would be useful,” Ostrosky-Zeichner says. “We need a systematic way to approach this, with a national registry.”There are some efforts to share treatment guidelines among physicians. The U.S. Centers for Disease Control and Prevention has interim guidance for treating patients with Long COVID, and several medical groups, like the American Academy of Physical Medicine and Rehabilitation, have released Long COVID treatment guidelines.
Rebecca Stumpf for TIMEMike Rausch takes a neurocognitive test to measure brain fogThis type of collaboration is also useful to patients navigating their new condition. One of Fitton’s biggest complaints is that Long COVID experts don’t always share their knowledge publicly, leaving patients on their own unless they can get into a specialty clinic. “Nobody seems to know what to tell me to do,” Fitton says. “I feel like answers are out there, and I’m just having to do my own advocacy.”Despite efforts to share best practices, some doctors still don’t believe their patients have Long COVID, which presents another barrier to treatment. Jackie Olvera, 38, experienced debilitating symptoms, including tremors and paralysis episodes, months after being hospitalized with COVID-19 in January 2021. But Olvera says that when she suggested to her doctor that she might have Long COVID, she was dismissed. “She told me to stop blaming COVID for all my symptoms,” Olvera says. “She told me that the only thing that was wrong with me was that I needed to lose weight and exercise.” Later, Olvera found a physician who agreed she had Long COVID and enrolled her in a specialty clinic near her home in California.The initial doctor’s reaction wasn’t only an obstacle to treatment. Olvera says the doctor also slowed down the application process when she sought disability benefits. Although Olvera did ultimately get disability benefits, they expired at the end of January. She has also been too sick to work and is currently without health insurance, which means she can’t afford many treatments, visits to her Long COVID clinic, or her nearly $10,000 in medical bills. Although she still struggles with reduced mobility, chronic pain, and fatigue, Olvera plans to return to her hospitality job to regain health insurance.The ordeal has been taxing mentally as well as physically. “I was feeling like I wasn’t getting anywhere,” Olvera says. “I was just feeling so broken, so left out, and [doctors] weren’t listening.” There have been times when she considered suicide, she says—something that research suggests is alarmingly common among Long COVID patients. Up to 28% of people experience depression symptoms at least 12 weeks after their initial COVID-19 diagnosis, according to one recent paper published in the Journal of Psychiatric Research. Survivor Corps also reports that almost 20% of its members have considered suicide, and Berrent says the group is “fielding suicide threats on a daily basis.”Some preliminary research suggests that because the virus that causes COVID-19 can affect the brain, it could have psychological side effects. But the simple fact of having Long COVID can also take a psychological toll. Nieset, from the Montana Long COVID clinic, says some of his patients feel guilty that they survived when so many people haven’t. Others struggle to find acceptance from doctors and loved ones or have a hard time adjusting to their new realities, which can look very different from before they got sick. Many people are too ill to work, or even to leave their homes for long stretches of time. Trying to resolve a complex, hard-to-treat illness can be stressful and isolating.Whatever the cause, Nieset says Long COVID patients need mental—not just physical—support. “I’ve never seen a phenomenon in medicine where I’ve actually heard patients talking the way [people in the] military would, dealing with PTSD and different things,” Nieset says.Duke’s Yamey stresses that while Long COVID is a health condition, it also needs holistic solutions. “It’s not just about the health issues,” he says. “There are also issues around employment and the need for social support and sick pay and making sure that people can access disability benefits. You need to take a truly psychosocial and biomedical approach.”For patients who have experienced compassionate Long COVID care, like Amber and Mike Rausch, the payoff can be huge. For a while, the couple thought they might never feel well enough to enjoy activities they loved like kayaking, biking, and hiking, which led to some “dark days,” Amber says. Now they’re getting back to many of those hobbies and feeling hopeful about the future.“If I could do anything,” Mike says, “it’s to ensure that the news gets out that this is treatable, and you can feel better.”